Abstract
BACKGROUND:
Femoral neck fractures are frequent in the elderly population and lead to high morbidity and mortality. Hemiarthroplasty is an established surgical procedure for displaced intracapsular femoral neck fractures. Post-operative infection is frequent and is potentially devastating for the patient and the healthcare services. The goal of this study was to identify the risk factors of infection after hemiarthroplasty and help adapt our surgical practice.
METHODS:
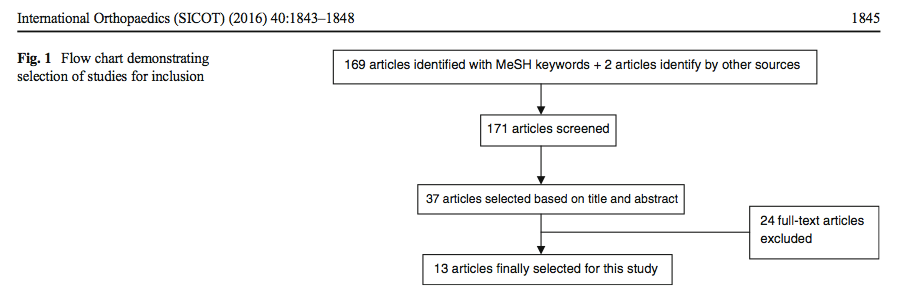
A systematic review of the literature was performed in July 2015 by two authors using the MedLine, PubMed and Cochrane databases. We used the MeSH keywords « hip hemiarthroplasty » AND « infection » to identify risk factors and methods of prevention for surgical site infection after hemiarthroplasty. Following the search, two authors independently performed the first stage based on titles and abstracts.
RESULTS:
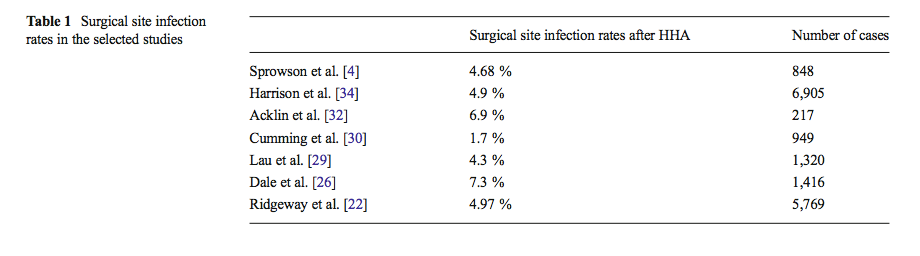
Thirty-seven articles were selected. Review and analysis of the references was performed to find other articles of interest. Thirteen articles were selected to analyse. According to literature, the surgical site infection (SSI) rate after hip hemiarthroplasty (HHA) is between 1.7 and 7.3 %. Pre-operative comorbidities (obesity, liver disease, advanced age), operative conditions (junior surgeon, uncemented stems, time of surgery) and post-operative management (length of hospitalisation, haematoma, prolonged wound drainage and two urinary catheterisations) were identified as risk factors of surgical site infection. Authors describe conditions to decrease the incidence of these complications and underline the importance of « a specialised hip team » that provides fast care and helps decrease the duration of hospitalisation.
CONCLUSIONS:
Careful patient management for hemiarthroplasty is vital and may decrease the incidence of surgical site infection, which is associated with high morbidity and high procedure cost. Our review suggests that there are specific correctable risk factors for SSIs after HHA. Being able to identify these risk factors leads to better care because of SSI prevention in patients undergoing HHAs after femoral neck fractures. To improve the outcomes, some methods of prevention of surgical site infection are available: before, during and after the operation.
STUDY DESIGN:
Review of literature.
LEVEL OF EVIDENCE:
IV.